Endometriosis
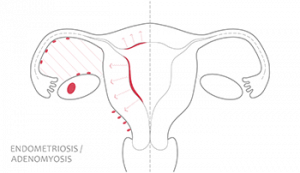
Endometriosis is a common condition suffered by many women in the reproductive age group. The cause of this condition is still unknown, although many theories have been considered. The most popular theory is that of retrograde menstruation, where menstrual blood “leaks backwards” from the womb into the pelvis, instead of the leaving the body via the vagina. As such, the active womb lining glands find their way into the pelvis and implant to cause endometriosis, commonly on the ovaries, womb surface, fallopian tubes, pelvic lining and even intestines. The presence of these tissues in the wrong part of the body is recognized by the immune system as “foreign”, which leads to chronic inflammation in the pelvis, resulting in permanent scarring with pain for some women and infertility for others.
The ideal treatment for endometriosis has yet to be found. The effective hormonal therapies have their own side effects, which may sometimes be more bothersome than the disease itself. These hormonal regimens seek to control the symptoms by reducing the lesions, but they invariably disrupt natural ovulation of the women and are thus counter effective for infertility treatment.
Surgery for endometriosis fundamentally aims to remove as much of the disease load as possible, allowing for faster symptomatic relief, without the detrimental effect on ovulation. However, such surgery requires proper training and technical proficiency to achieve the objective of removing the disease while avoiding damage to the surrounding structures, such as ureters, intestines and fallopian tubes. If the removal of endometriotic cysts of the ovary is to be undertaken, extra care must be taken to ensure that the maximum amount of eggs are conserved in the remaining ovary.
The selection of cases for endometriosis surgery should be individualized for every patient, depending on the objective of treatment, current status of disease and reproductive potential of the couple (including partner’s status), if fertility is the aim. Sometimes, the severity of the disease does not allow for complete removal, hence in such cases, hormonal therapy may be added on after surgery to achieve maximal therapeutic effect. Majority of such cases will require IVF to conceive eventually.
When surgery is successfully completed, those couples seeking fertility may be advised to attempt spontaneous pregnancy for a period of six to twelve months, beyond which assisted reproductive techniques may be considered. Repeat surgery is only offered in selected women, as it gets more difficult technically and the chance of successful clearance is lower.